Her dreams of further athletic achievement shattered, Frecklington heroically put the pieces of her life back together.
“One thing my accident taught me is that life is for living, so get out there and do it. That’s why I was in Spain. I gave myself a couple of years off – in the end I got six months,” she says.
A visit to a doctor in Spain confirmed the worst-case scenario – part of her metal implant had punctured through into her throat.
An initial surgery to correct it was abandoned halfway through when doctors realised how extensive the problem was.
“I went in for the surgery and they woke me up afterwards and said they hadn’t done anything because they didn’t have the facilities.
“They just put a feeding tube in me and told me they didn’t know how to fix me.”
Frecklington says she was discharged from the Spanish hospital in February 2020, and the hospital was shut down to non-urgent patients in March as the full force of the pandemic swept the country.
Living by herself away from major cities meant Frecklington was not at major risk of contracting coronavirus but her condition meant she was a high-risk case, and that, coupled with a desire to fix her ongoing condition, meant she wanted to come home.
It wouldn’t be easy.
The long way home
Frecklington is technically a New Zealand citizen, although she has lived most of her life in Australia, so getting home during the pandemic was made exponentially harder.
Her regular doctor in Cairns had recommended she see surgery specialists at the Princess Alexandra Hospital about her case, but getting back to Brisbane seemed almost as impossible as her medical issues.
Keri Frecklington several weeks after the surgery with her head brace and tracheotomy tube.
Having been overseas for several months, Frecklington was on a ticking clock as to whether her 12-month window to re-enter the country as a permanent resident was closing.
“They actually stopped me at the gate at Heathrow and said they had to call ahead because a flag had come up on my ticket,” she says.
“They told me it had been too long and I wasn’t allowed to re-enter Australia.”
Frecklington’s medical issues were deemed non-life-threatening, and with the pandemic forcing intake restrictions around the world, she was facing the prospect of living with a debilitating complication until it caused her a serious medical issue.
She comes close to tears when recalling that moment. “It’s fair to say I was feeling a bit abandoned at that point,” she says.
“It was just such a slow process, and it was even more difficult because all my hospital records were in Spanish, which apparently created all sorts of problems.”
Thanks to some lobbying by doctors back in Australia, Frecklington finally secured permission to come home, and touched down in Brisbane on July 15, 2020, where she was whisked straight to the PA Hospital for her mandatory 14 days in quarantine.
The physical journey was over but her surgery journey was just getting started.
Plan for success
When Adam Frankel first met with Frecklington, he promised they would share a coffee together when she was on the other side of her surgery.
Dr Frankel is an upper gastrointestinal surgeon with the PA Hospital, and was one of the doctors who worked to bring Frecklington home so she could have her life-changing surgery.
“Keri had a really complicated problem that required a lot of thought and pre-planning and multiple specialists in different fields,” he says.
“What had happened to her was a disaster, because when her metalwork punctured her throat it created a direct portal for saliva and food – the distinctly unsterile environment of the human throat – onto her vertebral column.”
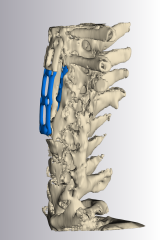
A 3D model of Frecklington’s neck vertebrae with the metal appliance in blue.
Dr Frankel rapidly organised a team of specialists via the Australian Centre for Complex Integrated Surgical Solutions, which was set up to deal with complex multi-disciplinary cases such as Frecklington’s.
They did imaging of her affected spinal area, created 3D-printed models to study, developed new implants to replace the old ones, and made meticulous plans for what would prove to be a marathon surgery.
“There’s a huge group of people behind something like this, and it requires a lot of thought, a lot of consideration of options, balancing the risks and benefits,” Dr Frankel said.
“It highlights the role of an organisation like ACCISS, where we have an in-house team that is used to dealing with complicated problems, so when we hear about a case like this, we’re ready to go.”
‘The most complex surgery I’ve seen’
Frecklington’s surgery took 20 hours, and featured 17 primary doctors as well as nurses and support staff.
First, the doctors had to ensure there was safe access to her airway to ensure she could remain under anaesthetic while surgeons were also operating on her throat.
“I don’t stress enough how difficult that is, to have access to her airway to keep her alive during the procedure but also have access to her spine behind her airway,” Dr Frankel says.
Surgeons then had to painstakingly remove the intricate metal supports that had been implanted in Frecklington’s neck a decade earlier, while avoiding further damage to the delicate muscles, nerves and blood vessels surrounding them.
Loading
After that, Dr Frankel says, they effectively had a “blank slate” to go in and replace the supports with new ones designed to fit Frecklington’s neck.
Cardiothoracic surgeons then had to split her ribcage to install further metalwork lower on her spine while avoiding her heart and lungs.
They then had to close everything back up, including repairing the initial hole in her oesophagus where the screw had first eroded through, causing the problem.
Doctors also took some muscle and skin from her leg to implant over the wound in her throat to give it a natural “cushion” during the healing process.
Dr Frankel says it was easily the most complicated surgery he has done.
“A 20-hour operation is pretty unusual and more unusual is having such a huge number of different specialty groups involved,” he says.
“You don’t want to make people worse as you’re trying to fix them.”
Time for a coffee
Frecklington spent six weeks with a tracheotomy tube in to allow her neck to heal. She also had a frame screwing her head and shoulders rigid so, in Dr Frankel’s words, “her head wouldn’t fall off” owing to the extensive internal work done.
Six weeks after the surgery, she had recovered enough to have that coffee with Dr Frankel.

Frecklington, flanked by some of the extensive team of doctors, nurses and technicians who performed her marathon surgery. Credit:Stuart Layt
“I remember very clearly the first day she arrived in hospital, I had to put all the PPE on for the COVID quarantine, I walked into her room and she said the thing she missed most was coffee,” Dr Frankel says.
“So it was amazing to go for a coffee with her just a few months after that.”
He said he was so happy to be able to get a good result for Frecklington.
“In other hospitals that didn’t have this degree of expertise, doctors might say it’s too difficult, and the solution then is to go home, you’ll never eat or drink again, you’ll be tube-fed for the rest of your life.
“When you’re a vibrant, fit woman in your 40s, that’s a disaster. So to be able to come up with a solution for Keri that has given her life back to her is a great outcome.”
For her part, Frecklington has already moved onto the next big challenge, moving again to Mount Isa and planning to get back into exercise, which she has kept up even after her first accident.
“I always say I’m the luckiest unluckiest person ever,” she says.
“I’m getting back to eating regular food, I can drink as much coffee as I want, I’m getting my life back.
“I took that for granted, even with my injuries. But I didn’t lose my voice, I didn’t need a tube, I didn’t need a tracheotomy for the rest of my life, and just thank them so much for that.”
Stuart Layt covers health, science and technology for the Brisbane Times. He was formerly the Queensland political reporter for AAP.
Most Viewed in National
Loading